1930 E. Rosemeade Pkwy #103 Carrollton, TX 75007
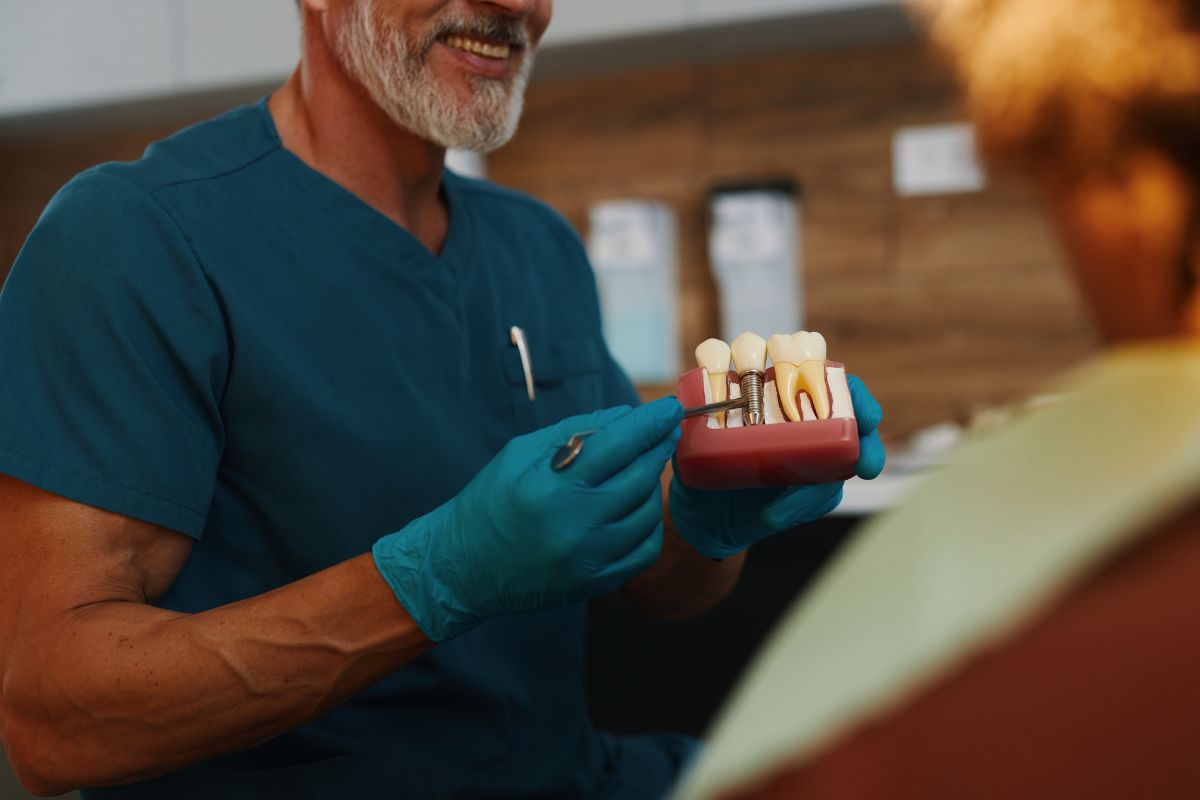
Dental implants are among the most reliable restorations in modern dentistry. It is designed to last for decades when properly cared for. Yet a surprising number of patients lose their implants far too early, not because of surgical failure, but because of dental implant maintenance habits that quietly do damage over time.
If you’ve already invested in restoring your smile, it makes sense to protect that investment with the same care. And if you’re considering a dental implant in Carrollton, knowing what to avoid from the start gives you a real advantage.
This guide walks through the five most common mistakes that shorten implant lifespans and what to do instead.
Why Dental Implant Maintenance Is Non-Negotiable
Unlike natural teeth, dental implants don’t get cavities. But that doesn’t mean they’re immune to damage. The titanium post fuses with your jawbone through a process called osseointegration, and that bond, along with the surrounding gum tissue and bone, needs ongoing care to stay healthy.
According to data published in the Journal of Dental Research, implant survival rates over 10 years exceed 95%, but that number drops when patients skip regular maintenance or develop habits that stress the implant’s structure. The difference between an implant that lasts 30 years and one that fails in 7 often comes down to what happens after placement.
Here’s what puts your implant at risk and what to do about each one.
Mistake #1: Treating Your Implant Like It’s Indestructible
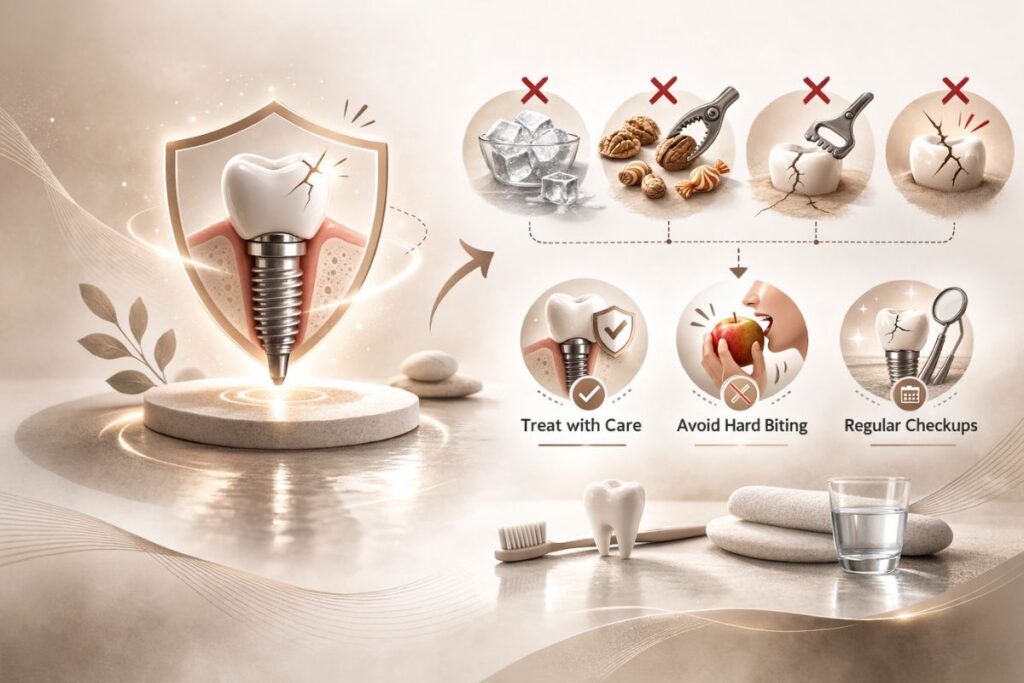
Patients sometimes assume that because implants are made from titanium and ceramic, they can handle anything. That mindset leads to habits like chewing ice, biting hard candies, cracking nuts with your teeth, or using your implant crown as you might use a tool. None of that ends well.
The crown sitting on top of your implant whether porcelain or zirconia can chip or crack under excessive force. Once the crown is damaged, the underlying abutment and post become vulnerable to bacterial infiltration and mechanical stress. Treat your implant-supported tooth with the same common sense you’d apply to your natural ones.
Mistake #2: Skipping the Floss Because It Feels Unnecessary
Here’s where many patients go wrong. Since implants can’t decay, some people stop flossing around them altogether. That logic seems reasonable until you understand peri-implantitis.
Peri-implantitis is an inflammatory condition affecting the tissue and bone around a dental implant in Carrollton and across the country, and it’s one of the leading causes of late implant failure. It functions similarly to periodontitis (gum disease) and is triggered by plaque accumulation around the implant base. The gum tissue becomes inflamed, bone loss begins, and the implant gradually loses the support it needs to stay stable.
A 2022 systematic review in Clinical Oral Implants Research estimated that peri-implantitis affects roughly 22% of implant patients – a figure that climbs sharply among those who don’t maintain consistent oral hygiene. Flossing with implant-specific floss or a water flosser, at least once daily, removes the bacterial biofilm that causes this condition before it takes hold.
Mistake #3: Ignoring Bruxism

Bruxism, the habit of grinding or clenching your teeth, often during sleep puts enormous pressure on implants. Natural teeth have a slight flex to them that absorbs this kind of force. Implants don’t. The titanium post transmits that pressure directly into the jawbone, which can lead to microfractures, loosening of the abutment screw, and crown damage over time.
Many people don’t know they grind their teeth until a dentist spots the signs. If you wake up with jaw soreness, morning headaches, or flattened tooth surfaces, bruxism may already be affecting your bite. A custom nightguard protects your implant from this kind of cumulative stress, and it’s one of the most straightforward ways to extend implant lifespan.
Carrollton sits in the heart of the DFW Metroplex, where many residents carry demanding work schedules and high daily stress levels. Not coincidentally, stress is one of the most commonly cited contributors to bruxism. If this sounds familiar, it’s worth raising with your dental team.
Mistake #4: Skipping Routine Dental Checkups
There’s a common misconception that once an implant is placed and healed, dental visits become optional. The opposite is true. Implants need professional cleaning and monitoring just as natural teeth do, arguably more so, because the warning signs of implant problems aren’t always obvious to patients.
During routine checkups, your dentist assesses implant stability, examines bone density around the implant with X-rays, evaluates gum health, and cleans areas that regular brushing and flossing can’t reach. Catching early-stage peri-implant mucositis, the inflammation that precedes peri-implantitis at this stage is far simpler than treating advanced bone loss.
Most implant patients should plan for professional cleanings every six months, though your provider may recommend more frequent visits based on your individual history. Skipping these appointments doesn’t save time; it borrows it from your implant’s future.
Mistake #5: Smoking After Implant Placement

Smoking compromises implant success in multiple ways. It restricts blood flow to healing tissue, slows osseointegration, reduces immune response, and creates an oral environment where harmful bacteria thrive. Research published in the International Journal of Oral & Maxillofacial Implants found that smokers face implant failure rates nearly twice as high as non-smokers.
This applies both during the healing phase and long after. Smoking after a successful implant doesn’t reverse the risks – it continues to weaken the gum and bone tissue that hold the implant in place. If you’re a smoker considering implants, or you’ve recently had one placed, talking with your dentist about cessation support is one of the most meaningful steps you can take for your long-term outcome.
Protecting Your Implant for the Long Haul
The practical takeaway from all five of these mistakes is the same: implant success is ongoing, not just surgical. What you do in the months and years after placement has as much influence on your outcome as the procedure itself.
A few habits that consistently support implant longevity:
- Brush twice daily with a soft-bristled toothbrush, electric is fine
- Use low-abrasive toothpaste to avoid surface damage on the crown
- Floss around the implant daily with implant-specific floss or a water flosser
- Wear a nightguard if you grind or clench
- Stay current on professional cleanings and radiographic monitoring
- Avoid tobacco in all forms
None of these requires dramatic lifestyle changes. Together, they create the consistent low-maintenance routine that keeps implants functioning well for decades.
Your Implant Is Worth Protecting – Let’s Help You Do That
At Flink Family Dentistry Carrollton, we work with implant patients at every stage – from placement planning to long-term monitoring. Whether your implant is new or years old, a checkup gives us the chance to catch anything that needs attention before it becomes a bigger problem.
Call us or request an appointment online. Protecting your implant starts with a single visit to our dental office.
People Also Ask
Yes. Late implant failure occurring a year or more after placement is typically related to peri-implantitis, excessive bite forces, or systemic health changes like uncontrolled diabetes. This is why long-term maintenance matters as much as the initial healing period. An implant that integrates successfully still requires ongoing care to stay that way.
Yes, electric toothbrushes are safe and often more effective than manual brushing for removing plaque around implants. Use a soft-bristled head and low-abrasive toothpaste. Avoid brushes with hard or medium bristles, as these can scratch the crown surface and irritate gum tissue over time.
Warning signs include pain or discomfort when chewing, swelling or redness around the implant site, a loose-feeling crown, or visible recession of the gum line around the implant. Any of these warrants a prompt dental evaluation. Some implant problems particularly bone loss are asymptomatic until they’re advanced, which is why imaging at routine checkups is essential.
Some medications can influence implant success. Bisphosphonates (used for osteoporosis), certain antidepressants, and immunosuppressants have been associated with altered osseointegration or healing. Always give your dentist a complete and current medication list before implant placement, and update them when medications change.
Not directly but the underlying factors that led to tooth loss (gum disease, bone loss, or certain systemic conditions) can continue to affect remaining teeth if unaddressed. Proactively managing the root cause reduces the likelihood of additional tooth loss over time.

